What is Perthes Disease?
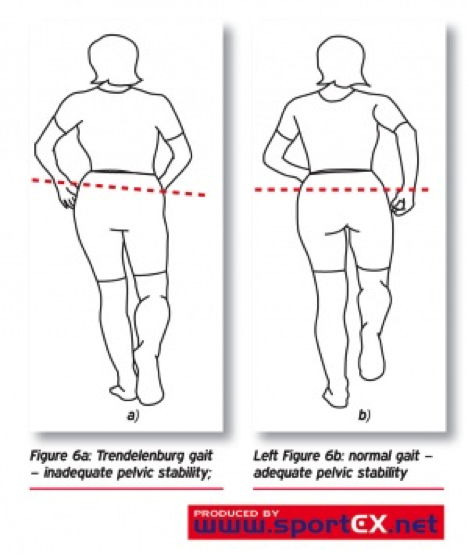
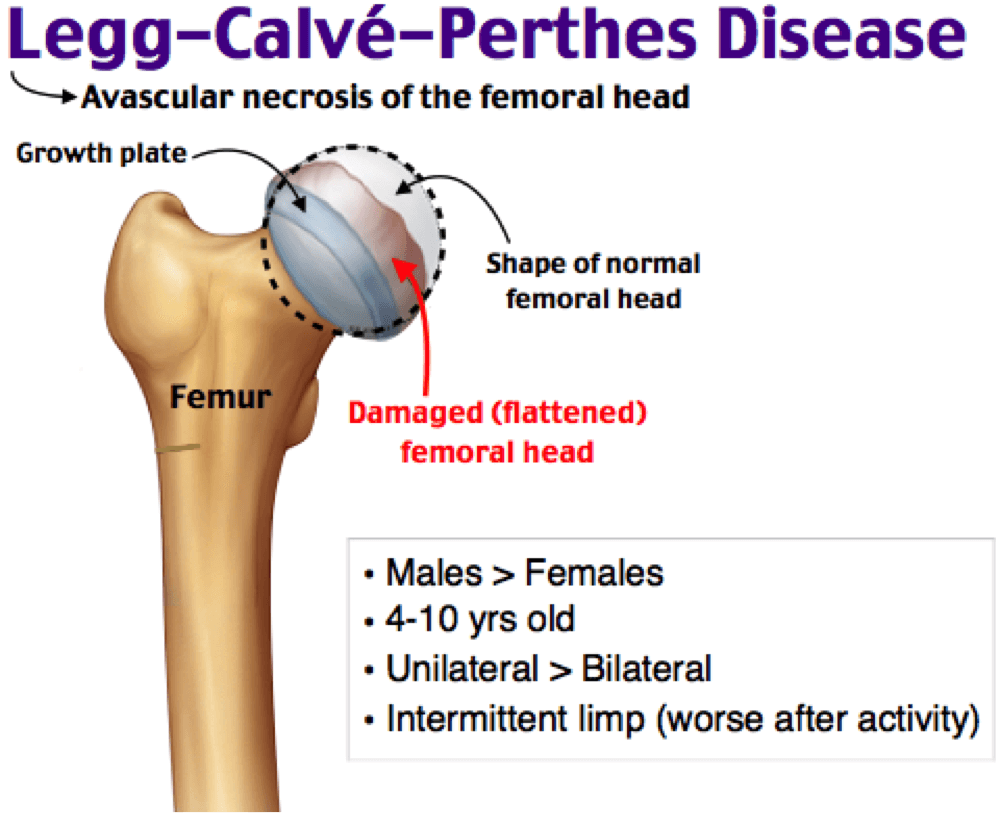
Perthes Disease, or officially termed Legg-Calvé-Perthes disease is a common condition affecting children ages 2-14. The disease manifests as bone death of the femoral head (ball) of the hip joint due to a loss in blood supply. Over time, this will cause the hip bone to necrose and ultimately deform. The pain felt is usually during the acute phases of the disease, with primary location of pain in the groin, hip or into the knee. Other features, apart from pain are abnormalities with walking or posture and atrophy in the leg and hip. Children will usually present with a limp that is worse after activity. (to avoid pain) gait patterns include a Trendelenburg gait and a Duchenne gait. (Pictured Right). Other common names for Perthes Disease include ischemic necrosis of the hip, coxa plana, oteochondritis and avascular necrosis of the femoral head.
What Causes Perthes Disease?
Unfortunately, there is no known cause. It is 5 times more common in boys than girls and reports have indicated that the incidence is higher in children in rural areas and of lower socioeconomic status. The presence of this disease will unfortunately lead to worse outcomes in adulthood, such as permanent deformity or commonly, early osteoarthritis in the hips. The prognosis of the disease will largely depend on the severity of pain as well as the age of onset. Children developing Perthes Disease later in childhood generally having poorer outcomes.
Most current theories suggest that mechanical strain on the hip will start the disease process. Subsequent loading of the hip then further impacts blood-flow to the femoral head. It has been found that hyperactive children are more likely to suffer from Perthes disease. Regardless of the cause of the disease, symptoms manifest similarly in all cases, with eventual bone death of the femoral head which leads to either a fracture due to the bone not being able to withstand mechanical loads, or bony deformations.
What should I do to avoid aggravating my Perthes Disease?
- AVOID activities that aggravate your pain, until you have seen your physiotherapist
- REMAIN ACTIVE, while avoiding aggravating activities.
- For RELIEF, applying ice to the area may help to reduce some pain and inflammation. Wrap the ice to prevent any direct contact with your skin
- RECEIVE physiotherapy care to get your joints, ligaments and muscles performing to their optimum level


